Hemodialysis is a method for cleansing blood from metabolic products. The hemodialysis procedure is carried out using the apparatus «Artificial kidney». The main indications are acute and chronic renal failure, poisoning of poisonous substances and drugs.
Content
Hemodialysis is a method of extracorporeal blood purification from the exchange products (mainly nitrogen bases) through an artificial semipermeable membrane of the device «Artificial kidney».
Indications for hemodialysis
Testimony for hemodialysis:
- Acute and chronic renal failure
- poisoning various poisons
- Poisoning medicinal substances
- severe blood electrolyte compound
In chronic kidney diseases, the testimony for hemodialysis is renal failure, which is not amenable to conservative therapy and goes into the terminal stage of the disease. Hemodialysis is a method that allows you to extend the life of the patient when the own opportunities for maintaining a satisfactory condition of the body are fully exhausted.
Symptoms of uremic intoxication arising due to an increase in the concentration in the blood of nitrogen bases are dyspeptic disorders (nausea, vomiting), the smell of urine in exhaled air, anemia, increased bleeding, dryness and yellowing of the skin, skin, sleep, and DR. The absolute sign of decompensated Uremia and the testimony for hemodialysis is considered pericarditis. Hemodialysis may be required in connection with the temporary deterioration of the kidney function, for example, due to the exacerbation of the underlying disease.
Contraindications for the use of hemodialysis
The use of software hemodialysis is contraindicated with patients with malignant neoplasms, lesions of the nervous system (hemiplegia), psyche disorders, some contagious (infectious) infections. An unfavorable conditions for hemodialysis are arterial hypotension, continuing internal bleeding and hemophilia.
Apparatus «Artificial kidney»
Hemodialysis is carried out using the device «Artificial kidney». The basis of its work is the principles of dialysis, allowing to remove a substance with a small molecular weight from the blood plasma (electrolytes - sodium, calcium, potassium, nitrogen - urea products, creatinine, urinary acid, etc.), and partially ultrafiltration, with the help of which excess water and toxic substances with a higher molecular weight are derived.
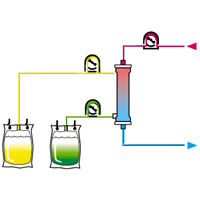
Despite the variety of structures, all artificial kidney devices have one diagram and consist of a dialyzer, a device for preparing and supplying a dialyzer solution, a perfusion device that provides blood progress through a dialyzer, and monitor.
The dialyzer is the main part of the apparatus. The most important functional element it is a semi-permeable dialysis membrane, which separates the internal space of the dialyzer into two parts for blood and the solution.
The dialysis solution of the composition is close to the ultrafiltrator of blood plasma and is intended to restore uremic disorders of the salt and acid-base composition of blood.
Hemodialysis procedure
During the hemodialysis procedure, the doctor uses access for blood through hemodialysis. The function of the apparatus is to output the products of exchange and regulate the plasma chemical balance. After that, the purified blood returns to the bloodstream through hemodialysis access. Creating an access - port, is a small operation. There are two types of ports. The most common access is fistula (artery compound with veins) and stent (artificial tube, which connects the artery with Vienna).
A week after the operation fistula starts «ripen». It increases in size, it may look like a cord under the skin. The whole process usually takes 3-6 months. Ripe fistula should be wide and enough elastic so that it can be easily introduced into it dialysis needles.
The stent can be used 2-6 weeks after his adheated occurs. Typically, preference is given to the fistula, since it is used to form their patient's own fabrics, which are more resistant to infection than the stent. However, when the veins of the veins or their small diameter, the preference is given to the Stat.
When used, both fistulas and stents, the connection between the artery and the vein increases the volume of blood flow through vein. In response to this vein stretches and becomes elastic. Due to this, a greater amount of blood passes through Vienna, which increases the effectiveness of hemodialysis.
Before carrying out the procedure, an artificial kidney apparatus is sterilized and washed, connected to a canister with a dialysis solution.
The duration of hemodialysis is approximately 5-6 hours. In the course of the procedure, doctors keep continuously monitoring arterial pressure, patient pulse and other indicators, as well as for the state of vascular access. At the end of the procedure on the area impose aseptic (sterile) bandage.
Complications of hemodialysis
The kidneys participate in the work of many systems in the body therefore, when the kidneys cease to work, the function of other body systems is also violated. Unfortunately, this leads to a violation of the work of the whole organism and affects the patient's state. Complications of hemodialysis:
- anemia
- Bone diseases
- Arterial hypertension
- pericarditis
- Increased potassium level
- Defeat of the nervous system
Anemia
Anemia means that the amount of red blood cells (red blood cells) decreases in the blood, which with the help of hemoglobin tolerate oxygen in the tissue. Among the causes of anemia during dialysis are distinguished:
- The lack of erythropoietin, hormone produced by healthy kidneys to stimulate the formation of erythrocytes in the bone marrow
- Bloodstocks due to bleeding, dialysis and blood fences
- reduced iron consumption and vitamins with food due to diet, poor absorption of iron in the intestine or loss of iron and vitamins during dialysis
Bone diseases
In patients with a terminal phase of renal failure, the absorption of calcium, phosphorus and vitamin D is disturbed. This leads to increased fragments of bones (renal osteodistrophy). As a result of these changes, osteomalization appears (bone destruction) since the kidneys cannot turn vitamin D into a form that facilitates calcium suction. Balance of calcium and phosphorus in the blood in the blood leads to the deposition of substances in the heart, lungs, skin, vessels and joints. Calcium deposition in the skin leads to the appearance of inflammation, the development of painful skin ulcers (calcifylaxia).
Enhance arterial pressure
If there is an increased blood pressure together with a disease of the kidneys, it should be limited to the use of cook salt and liquid. If arterial hypertension is not treated, the damage to the vessels can lead to the development of stroke or heart attack.
Pericarditis
Pericardite is called inflammation of the shell covering the heart - pericardium. The main reason is the lack of dialysis. The accumulation of fluid around the heart occurs, the ability of the heart is disturbed and blood release decreases and decreases.
Increased blood potassium level (hypercalemia)
Patients with hemodialysis recommended a low-mains diet. Increased blood potassium can lead to a heart stop.
Damage to the nervous system (peripheral neuropathy)
Peripheral neuropathy is manifested by impaired sensitivity in the area of brushes, stop and legs. This happens for various reasons, among them the accumulation of productivity products of the body, diabetes, lack of vitamin B12 and other reasons.
Prevention of the development of complications during hemodialysis
The final decision on the duration of the treatment and prevention of complications is assumed by the patient. Measures for the prevention of the development of complications include:
- Preventing infectious complications in the observance of hygienic requirements for intravenous catheter
- Compliance with the diet appointed doctor
- Eating recommended fluid volumes
- Receiving assigned drugs
- According to the treatment plan, hemodialysis in specialized centers
- report to the medical staff about all the symptoms of complications
If hemodialysis is required for the treatment of the terminal phase of renal failure, then recommendations and appointments of medical staff should be carried out to prevent complications.