What is a bubble uretera reflux? How the bubble ureteral reflux is manifested? How to diagnose and how to treat bubble and ureteral reflux? Read in this article.
Content
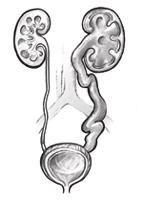
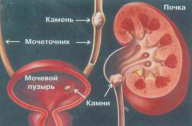
Bubble-ureteral reflux (PMR) - Anti-Bladder Purpose Anti-Bladder Rights.
In children's practice PMR – One of the most frequent reasons for secondary kidney wrinkles with a function loss. First, the reverse urine current does not provide complete evacuation of microflora penetrating into the urinary routes, which leads to chronic kidney inflammation (pyelonephritis). Secondly, at the time of the deployment of urine into the kidney pelvis, the pressure in it repeatedly increases, which leads to mechanical damage to the renal tissue. The outcome of chronic inflammation and excess hydrodynamic load is the scarring of renal tissue with a function loss (secondary kidney wrinkling, nephrosclerosis).
There are 3 main causes of the emergence of the PMR. All of them lead to the insufficiency of the valve function of the intrapaulic ureter. The most common in children – Congenital anomaly of the ureter's mouth. Second – Increased pressure in the bladder due to impaired function or obstacle in the urethra. Third – Chronic cystitis, in which the elasticity of the fabrics of the intrapaulic ureter is disturbed.
Manifestations of bubble-ureteral reflux
Occasionally there are complaints of abdominal pain or lumbar field of defeat. But most often, the bubble-ureter reflux does not show itself clinically to the development of pyelonephritis. The latter has a characteristic clinical and laboratory picture, well-known pediatricians. In the acute phase of the disease, high temperature is marked, symptoms of intoxication. In urine analyzes, the number of leukocytes increases, protein appears. In the blood tests, an increased level of leukocytes is also determined, an enlarged. As a rule, children with acute pyelonephritis pediatricians are sent to inpatient treatment, after which the urological profile is usually conducted.
Methods of examination with bubble-uretera reflux
The main method of diagnosing PMR is cystography.
Cystography – X-ray study to estimate the anatomy of the bladder and the urethra, to identify the bubble-ureter reflux (cast urine from the bladder in ureters).
Research methodology: in the bladder through a catheter conducted by the ureage channel, a water-soluble contrast agent is injected before the urination appearances appear. 2 shots are produced: first – Immediately after filling the bladder, the second - during urination. For boys, the second shot is performed when turning the pelvis in 3/4 for visualization in the images of the urethra throughout. For the prevention of urinary tract infection, research is carried out under «Cover» Antibiotics.
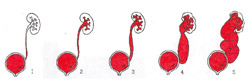 There are 5 PMR degrees. Classification criteria is «height» Purple of urine and the degree of ureter expansion.
There are 5 PMR degrees. Classification criteria is «height» Purple of urine and the degree of ureter expansion.
In addition to identifying the reflux itself, the determination of its degree, it also allows you to obtain the information of the urethra's accountability and suspect the violation of the bladder function.
Additional information on the state of urinary organs in children with PMR allows you to obtain intravenous urography, explorer the function of the bladder, cystoscopy and laboratory tests. The residual function of the affected kidney is determined on the basis of a radioisotope study, since with a critical violation of the function, the elimination of reflux is not always appropriate and the optimal help of the patient may be removal of kidney.
Treatment of bubble-ureteral reflux
Methods of treating different forms of PMR differ from each other. In the primary reflux arising against the background of the anomaly of the ureter's mouth, it is necessary to effect on the output of the ureter (surgical or endoscopic interventions).
In secondary PMR, diseases leading to their occurrence (treatment of cystitis, urinary bubble dysfunction, regeneration of the urethra dysfunction).
The form of reflux is specified in cystoscopy at the state of the ureterals. Therefore, to choose the right tactics of treatment, you must examine the child in a specialized urological hospital, which has extensive experience in the field of urological endoscopy.
Surgical methods for the treatment of bubble-ureteral reflux
 To date, in most Russian urological hospitals, surgical treatment of bubble-ureteral refluxs is practiced. The task of all antirefluux operations is to create a sufficiently extended submembiatricular ureter department. At the same time, the urine, filling the bladder, presses the elastic upper wall of the ureter to the bottom, lying on a rather dense muscular bladder layer, which provides the valve antirefluxual function.
To date, in most Russian urological hospitals, surgical treatment of bubble-ureteral refluxs is practiced. The task of all antirefluux operations is to create a sufficiently extended submembiatricular ureter department. At the same time, the urine, filling the bladder, presses the elastic upper wall of the ureter to the bottom, lying on a rather dense muscular bladder layer, which provides the valve antirefluxual function.
Despite the high efficiency of surgical interventions, they all have significant disadvantages: high trauma, the need for long-term combined anesthesia. For the free outflow of urine in the postoperative period, urinary tracts should be mandatory temporarily drained with tubes, which are derived from the skin. The first days after surgery, children are carried out in resuscitation departments, as there are intensive therapy and drug anesthesia need. The duration of even the uncomplicated hospital period after a long-term operation is depending on the nature of the interference of the intervention from 14 to 30 days.
The possibility of early and late postoperative complications should also be taken into account, such as bleeding, aggravation of pyelonephritis, scar narrowing of the anastomosis (place of crosslinking the ureter with bladder), recurrence of bubble-ureteral reflux. The last 2 complications suggest repeated operations on the ureters, which under the conditions of barking tissues are much heavier and the effectiveness of them lower than the primary.
Endoscopic treatment of bubble-ureter reflux
The essence of the method is to restore the impaired antirefluxic function of the ureter by administering under its output of the liquid inert («indifferent» for human tissues) polymer. The polymer forms a tubercle, which, after frozen, serves as a rigid support for the ureter, the top wall of which, tightly adjacent to the bottom, provides the valve antireflux function.
Intervention is carried out during cystoscopy, under short-term inhalation (mask) or intravenous anesthesia. The duration of the procedure is an average of 10-15 minutes. The severity of intervention is determined how easy the child is tolerates anesthesia. As a rule, after 2-4 hours, the patient's condition is fully normalized. After 3-5 days, children are discharged under outpatient surveillance. Before discharge, antibacterial prophylaxis of pyelonephritis is carried out.
The control examination is carried out in 3-6 months. When recurrence, the PMR is re-endoscopic intervention. Up to 85% of patients get rid of the PMR after the first procedure.
Thus, high efficiency at low traumatism, in our opinion, determines the priority position of endoscopic interventions in relation to antirefluux operations. A small part of the patients in whom the PMR is a fearless endoscopic way can be operated on without technical difficulties associated with preceding endoscopic treatment.