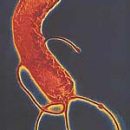
Etiology, classification, clinical picture, diagnosis and treatment of acute myeloid leukemia.
Content
 Sharp leukemia — Heterogeneous group of clonal
Sharp leukemia — Heterogeneous group of clonalTumor diseases of the hematopoietic fabric characterized uncontrolled
proliferation, disruption of differentiation and accumulation in the bone marrow and
peripheral blood of immature hematopoietic cells.
Acute leukemia is 2-3% malignant tumors
man. The incidence of sharp leukemia is an average of 3-5 cases on
100,000 population. In 75% of cases, the disease is diagnosed in adults, 25%
Cases — in children. The average ratio of myeloid and lymphoid sharp leukemia
is 6: 1. In adult patients over the age of 40 years of 80% of cases
presented by myeloid forms, in children — 80-90% — lymphoid. Median
age patients with acute nonlimfoblastic leukemia — 60-65 years old, sharp
lymphoblastic leukemia — 10 years.
There is a genetic probability of developing acute
Myeloid Leukoza. There are a large number of family cases reports
Diseases, the likelihood of an IML for the nearest relatives of the patient
three above. A number of innate states can
increase the likelihood of Oml. Most often it is Down Syndrome, in which the probability of an IML is raised in
10 — 18 times.
Some carcinogens
(causing tumors agents) can be considered as etiological factors
OML, such as gasoline, smoking tobacco and ionizing radiation. Most important
Risk factor is older than 65 years.
The influence of individual
The genetic features of the body, as well as the impact on the body of exogenous
Factors manifests itself in the development of secondary acute myeloid leukemia,
components of 5-20% of all cases of IML. In particular, the IML may develop
People previously undergoing treatment with various chemotherapy modes
Other malignant formations.
The presence of the preceding phase in
the form of myelodsplastic syndrome (MDS) most common in the elderly
patients, too, is an important risk factor Oml. Antitumorian
Chemotherapeutic effects, especially alkylating drugs, anthraciklines
and epipodophillexins, increases the probability of the development of secondary
OML / secondary MDS. The highest probability of the disease falls for 3-5 years
After chemotherapy. Combined application of chemo / radiation therapy is also significantly
Increases the risk of secondary IML / secondary MDS. It should be noted that secondary
leukemia / MDS arise not in all patients receiving antitumor
treatment.
Acute leukemia is
Consequently damage — Mutations — In the genetic material of the clone
Hooping cell. As a result, the molecular level occurs
Events leading to a violation of control over the cell cycle, change
Transcription Processes and Products of a number of key proteins-regulators. Malignant
Meloblasts protrude cells with OML,
incapable of ripening and differentiation as a result of impaired
genetic control and accumulating
in bone marrow. Lakeclone cells
interfere with the activities of normal cells, pushing them from bone marrow.
Currently all sharp
leukemia is taken to divide on myeloid and sharp lymphoblastic leukemia.
The classification of the WHO sharp myeloid leukemia is presented below.
Classification of WHO sharp myeloid leukemia
| Name subspecies | Description |
|
Oml S characteristic genetic changes |
In patients with such a subspecies of the IML Usually high levels of remission and the forecast is better comparatively with the OML of others subspecies. |
|
Oml with dysplasia Several Rostkov |
This subspecies Includes patients with preceding myelodsplastic syndrome (MDS) or myeloproliferative disease (MPB), which go to the IML. This subspecies of the IML is more common in the elderly and Differs unfavorable outlook. |
|
Oml I MDS associated with previous treatment |
This subspecies OML includes patients receiving chemistry and / or radiation treatment after which came the IML or MDS. With these leukemia, there may be characteristic Changes in chromosomes, the forecast for them is often worse. |
|
Oml, N subject to the signs of listed subspecies |
Includes Oml subspecies that are not included in those listed above. |
Franco-American-British
classification
Franco-American-British classification (Fab)
The system shares an IML to 8 subspecies, from M0 by M7, based on the types
cells — leukocyte predecessors, and on the degree of maturity of the changed
cells. Determination of malignant cells are carried out on the basis
external signs with light microscopy and / or cytogenetically, detecting
underlying deviations of changes in chromosomes. Different subspecies of the IML
Different forecast and response to treatment. Despite the advantages of the WHO classification,
Fab system is still widely used. By Fab there are eight subtypes
Oml.
| Subspecies | Name | Citogenetic changes |
| M0 |
Minimally differentiated Acute myeloblastic leukemia |
|
| M1 |
Spicy Myeloblastic leukemia without ripening |
|
| M2 |
Spicy Myeloblastic leukemia with ripening of granulocytes |
T (8; 21) (Q22; Q22), t (6; 9) |
| M3 |
Promelocyrtar, Or acute promelocyrtar leukemia (op floor) |
t (15; 17) |
| M4 | Spicy Myelomocytic leukemia |
Inv (16) (P13Q22), DEL (16Q) |
| M4EO |
Myelonocital Combined with bone marrow eosinophilia |
Inv (16), t (16; 16) |
| M5 |
Acute monoblastic leukemia (M5A) or acute Monocystary leukemia (M5B) (M5B) |
DEL (11Q), t (9; 11), t (11; 19) |
| M6 |
Spicy erythitoid leukemia, including erythrocytarian leukemia (M6A) and very rare clean Erythitoid leukemia (M6B) |
|
| M7 |
Spicy Megakaryoblastic leukemia |
T (1; 22) |
| M8 |
Acute basophilic leukemia |
Clinical picture
The clinical picture of acute leukemia is determined by severity
Basic syndromes:
-
Anemic — reduced hemoglobin levels and
the number of erythrocytes, which manifests itself
weakness, decrease in working capacity, drowsiness, manifestations
heart failure, heartbeat,
weakness, shortness of breath, pallor of skin and mucous membranes, orthostatic
hypotension, secondary angina and myocardial infarction, intelligent
Chromota, clinic of respiratory failure in patients with chronic
Broncho-pulmonary diseases (COPD). -
Granulocyteopenic — Infectious complications,
due to a decrease in the number of granulocytes in the blood, which is manifested by high temperature and intoxication, as well as
Local clinic (necrotic districts, ulcerative stomatitis, osteomyelitis
Jaws after the extraction of the tooth) or generalized (sepsis, infectious endocarditis),
more often bacterial, infection. -
Hemorrhagic
— Hemorrhage in skin and mucous, nasal and gum bleeding,
Gastrointestinal and renal bleeding, uterine bleeding, elevated
Bloodfaction during operational interventions. -
Proliferative
— Lymphadenopathy, Splenomegaly, Hepatomegaly, Hyperplastic Gingivitis,
Pains in the bones, disorders of the function of the cranial brain nerves, headache, violations
vision, general and focal neurological
symptomatics, headache, priapism. -
Inxication
— Weakness, decline in appetite, weight loss, sweating.
Diagnosis of sharp leukemia
 First
First
Step in diagnostics is
Clinical analysis of blood by taking blood sample from veins. In blood sample
The number of blood cells (erythrocytes, leukocytes and their subtypes is determined, and
Also platelets). When discovery in clinical analysis of blood more than 20%
Blast cells can be diagnosed with acute leukemia.- At
the absence of sufficient blood to diagnose the number of blasts, as well as
The purpose of accurate verification of the diagnosis using additional methods
Studies are shown to conduct an aspiration biopsy of the bone marrow.
The study of the bone marrow includes a study of bone marrow aspirate
(Analysis of my cellogram-cytological examination), in rare cases, spendpalobiopsy is carried out
bone marrow for a histological study of the bone marrow. - IN
quality of additional research methods to determine the variant of acute
leukemia and prognostic markers are carried out:
-
Cytoochemical
Research (myeloperixidase, eserase, glycogen) -
Cytogenetic
study — detection of chromosomal anomalies, such as absent or
Additional chromosomes in bone marrow cells by standard analysis
Metafaz or FISH method
(Fluorescent
In. hybridization
situ — Method based on the ability
chromosomal DNA (target) to contact under certain conditions with small
DNA sequences (probes), complementary this chromosomal DNA. At
Accession to the fluorescent substance probe produce DNA analysis by its
location of cells in interphase cells). The results of cytogenetic
Studies are worn both diagnostic importance and prognostic.
| Exodus | Deviation | 5-year survival | Recurious frequency |
| Favorable |
T (8; 21), T (15; 17), inv (16) |
70% | 33% |
| Satisfactory |
Not Revealed, +8, +21, +22, Del (7Q), DEL (9Q), violations 11Q23, all other Structural or Numerical Changes |
48% | fifty % |
-
Molecular biological
research (genetic research is carried out to identify characteristic
mutations that can affect the outcome of the disease — For example, FLT3-tyrosine kinase, CD117 gene, retired for the receptor synthesis
Stem cell growth factor C- Kit, Cebra genes,
Baalc, ERG, NPM1. -
Study
On tumor cells of differential antigens (CD) by flow cytometry (immunophenotyping).
In the future in patients with sharp
leukemia re-studies of bone marrow in order to
Determine the effect of therapy, the completeness of the remission achieved and the process stage
(remission, stabilization, progression).
Clinical stages and phases of the disease
-
Primary-active
stage — time interval between first clinical manifestations
Diseases, diagnosis and the first full remission -
Full
Clinical hematological remission — The number of blast cells in myelogram
Decreases less than 5%, there are no extra-visa leukemic foci
lesions, while in peripheral blood should not be blast cells,
Number of platelets 100×109 / l leukocytes 2.5 x
109 / l, granulocytes 1.0 x
109 / l, hemoglobin level of 100 g / l.
Recently, the concept of cytogenetic and molecular biological
remission. -
Stage
minimum residual (residual) disease. -
Recurd
Diseases (bone marrow, extraotic surge). -
Terminal
stage.
Treatment
Before starting treatment, a complete clinical
Patient examination to assess the state of concomitant pathology
Cardiovascular, respiratory, urogenital systems, central nervous system.
It includes a complete biochemical blood test, coagulogram, examination on
Hepatitis B and C, HIV, Viruses of the Herpes Group. Ultrasound of organs
Abdominal cavity, chest x-ray study / Computer
Tomography of chest, ECG / Echo Cardiography, CT / MRI head, inspection
neurologist, oculist and t.D. All this is necessary for the right choice of treatment and
Preventing complications.
Treatment methods
Patients with IML depend on the type of disease, prognostic factors, age
the patient, as well as related pathology and can be divided into
Potentially healing therapeutic methods and supporting therapy.
Supporting I
Symptomatic therapy
Foundation
OML treatment is supportive therapy, which includes the treatment of intercurrent infections, uricultural
diathesis, replacement therapy with blood components, as well as treatment
Concomitant pathology.
Based on
Supporting therapy of patients with MDS lies replacement therapy
Blood components. Patients with low risk of development Oml anemia can be
Main clinical meaningful problem. Replacement therapy
facilitates symptoms of anemia and, therefore, is an important treatment.
Frequency
transfusions depends on the state of the patient, the severity of anemia, as well as
concomitant pathology, especially the need for overflowing components
blood when developing in patient bleeding. The result of substitution therapy
is an increase in hemoglobin level, which studies show,
has a positive correlation with a quality quality indicator.
Transfusion
platelet mass is carried out in cases where the number of platelets
extremely low and / or there are hazardous bleeding. Under development
Coagulopathy (violations in the blood coagulation system, for example, level reduction
Fibrinogen or prothrombin complex factors) conduct replacement
Therapy of blood plasma components or
recombinant prepartes (Novosvlen, PromromBoplex and PR.)
Potentially healing therapeutic methods
-
 To control the symptoms of the disease or cure of the IML in young patients use
To control the symptoms of the disease or cure of the IML in young patients use
Intensive chemotherapy to destroy the clone of pathological
cells and reach long remission. This treatment method has
Significant side effects, such as hair loss, the appearance of stomatitis
oral cavity, nausea, vomiting, appearance of liquid stool. In addition to these side
phenomena, chemotherapy has adverse effects and healthy
cells that require a long stay in hematological
Departments. At this time, the patient is carried out over-blood cell and
thrombocyte mass, antibacterial drugs are prescribed to combat
infection. If induction chemotherapy provides adequate control over
pathological cells (state of remission), then restoration of normal
Blood cells should begin within a few weeks. However, even in cases
Successful treatment disease can be returned — recur. - The only one
known method of treatment capable of healing most patients with OML,
is the transplantation of allogeneic (donor) hematopoietic stem
cells. It should be borne in mind that this is a complex risk-related procedure
early and late complications. The outcome of treatment depends on the degree of compatibility (HLA compatibility) of the donor and the patient
(recipient), as well as on the availability of suitable donor cells (availability
Compatible blood brothers and / or sisters, availability of donor bank). Thus
The way there are strict testimony and contraindications for this type of treatment:
It is suitable for those cases when patients are able to transfer
Stem cell transplantation and have a suitable donor and answered chemotherapeutic treatment. - Study
The mechanisms of development of MDS / secondary IML, undertaken in recent years showed,
that for this pathology is characterized by hypermetilization of the promoter region
some genes-oncosuppressors, which leads to «Silence» These genes I
Proliferation of tumor cells and transformations in the IML. On the basis of these knowledge
The so-called hypometaling agents that contribute were developed
DNA hypomettylation, causing expression earlier «Disabled» Genov.
In May 2004, management
USA for food and drug control (Food and Drug Administranion, FDA) issued permission to use
Injection preparation Azacytidin (Vaidaza) for the treatment of all types of MDS. In the Russian Federation
The drug was approved for use in 2010, including for the treatment of both MDS and IML. The results of the study showed that
Azacytidin reliably prolongs life to patients with acute myeloid leukemia,
Scheduled stem cell transplantation / intensive
chemotherapy. The studies show that the survival rate of patients with an OML without modern treatment is 1.6
months, while Azacytidin increases lifespan with IML
11.1 months, possessing favorable
Safety profile. Besides,
the drug, with sufficient qualifications of medical personnel, may
Apply Ambulator.
According to the protocols adopted in Russia, the treatment of patients IML, which are not
Suitable for intensive
chemotherapy and secondary OML is carried out by low doses of cytarabine and / or with
using supporting therapy [one]. Such therapy
Improves the quality of life of patients, but does not increase their life
in comparison with the natural course of the disease. While use
Azacitidine in this category of patients can radically change the flow
Diseases (Table 1).
table
one. The average total survival in the patients of the IML, depending on therapy (indirect
Comparative data).
| Without treatment | Supporting therapy | Low doses of cytarabin | Azacytidin | |
|
Oml, including number Oml S The number of blasts in myelogram 20-30% |
1,6 | 13,4 | 17.0 | 24.5 |
Median survival of patients with OML (20-30% of blasts),
receiving azacytidine, increases to 24.5 months. At the same time, the differences in the group
Azacytidine with groups of supporting therapy and low doses of cytarabin
statistically reliable (p = 0.045), regardless of age or karyotype, and
Optional months of life are 11.1 and 7.5 respectively (median
survival in the supporting therapy group equals 13.4 and in the low group
Doses of cytarabin — 17.0 months) (analysis of data research III phase AZA-001) [2]. After 2 years, 50.8% of patients in the group were alive
Azacitidine, which is 2 times more than in comparison groups (26.2%). For
Comparison — Patients with an OML who do not receive modern therapy (natural
The course of the disease) die within 7 weeks from the diagnosis.
 For patients with an IML, not
For patients with an IML, not
Intensive chemotherapy / stem cell transplantation, treatment
azacytidine may be the only means of life prolonging and
helping to achieve long remission. In the AZA-001 study in the Azacitidine group to therapy response
(Criteria IWG
2000) reached 29% of patients (full and partial answer), 49% — achieved
Hematological improvement. Differences with comparison groups («Supportful
therapy», «Low doses of cytarabin») Statistically reliable (5 and 12%, 31 and 25%
respectively). Time to the progression of the disease was 14.1 months in
Group «Azacytididine» and 8.8 months in comparison groups (p = 0.047). Duration
The hematological response was 13.6 months on the azacytidine in comparison with
5.2 months on traditionally used therapy (p = 0.002).
In patients with MDS and IML who received
Therapy ascitidine was observed a higher probability of independence from
Transfusions of the erythrocyte mass: 45% of patients became independent from
Hemotransphus, while on traditional modes — Only 11% (P < 0.0001).
Thus, the treatment of ascitidine of patients Oml (20-30% of blasts)
accompanied not only by a higher life expectancy and total
Remissary frequency compared to supporting therapy and low doses of cytarabina,
but also higher hematological improvement and independence
Transfusions. Patients with MDS High Risk Azacytidine Therapy
accompanied by an increase in time before transformation into an OML (17.8 months VS 11.5 months, p<0.001).
Azacytidin is included in the International Protocols for Treatment
Patients with myelodsplastic syndrome and IML in patients over 60 years.
USA: in the National Oml Treatment Guide
Oncological network (National Cancer Comprehensive Network, NCCN, USA) (2010) Azacytidine is recommended for application
patients older than 60 years who are not candidates for highly visible
Chemotherapy. Recommendations are given with a high level of evidence.
TO
undesirable phenomena of 3-4 degrees developing against the background of the treatment of azacytidine,
treat hematologic (71.4%), including thrombocytopenia (85%), neutropenia
(91%) and anemia (5