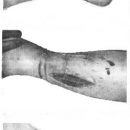
What are the wounds from bites? What are the dangers for health these injuries? Diagnosis and treatment of wounds.
Content
Appeals about busting wounds are quite frequent in outpatient surgical practice. The branched wounds are usually contaminated by various microorganisms, which can lead to an infectious process and, in the absence of medical care, the development of such complications, as a local abscess, osteomyelitis, septic arthritis, meningitis, remote abscesses and sepsis. Infection proceeds the most difficult in patients with immunodeficiency states.
Wounds from ukuusov
Man. Wounds after the bite of a person can occur during physical violence (for example, when skin damaged with teeth when hitting the jaw) and in the process of sexual contacts (the so-called «Love bites»). The bites are localized mainly on the fingers or arms, less often in the neck, chest, genitals. About 30% of the abrasion on the brushes caused by the blow of the teeth are accompanied by deep damage and the development of the infections of the ligament and bones, especially at the later (later than 24 hours) of medical care. Bacteria, contaminating wound, are represented by streptococci, Staphylococcus aureus, Homophiles SPP., Fusobacterium SPP., Bacteroids and other anaerobas, as well as Eikenella Corrodens. Infection with viruses, such as the hepatitis B virus, the hepatitis C virus and HIV, is observed significantly less.
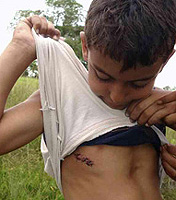 Dogs. Wounds after dog bites are contaminated by microflora animal data cavity, typically including such pathogens as Pasteurella SPP., Streptococci, staphylococci, anaerobic bacteria, and in 2-30% of cases are accompanied by the emergence of infection. Capnocytophaga Canimorsus, a gram-negative stick, occasionally a contaminating doggy (and feline) bites, can lead to a rapid development of potentially deadly septic syndrome, especially in immunocomplete. With the bite of a stray dog it is necessary to remember the possibility of infection with rabies.
Dogs. Wounds after dog bites are contaminated by microflora animal data cavity, typically including such pathogens as Pasteurella SPP., Streptococci, staphylococci, anaerobic bacteria, and in 2-30% of cases are accompanied by the emergence of infection. Capnocytophaga Canimorsus, a gram-negative stick, occasionally a contaminating doggy (and feline) bites, can lead to a rapid development of potentially deadly septic syndrome, especially in immunocomplete. With the bite of a stray dog it is necessary to remember the possibility of infection with rabies.
Cats. Feline bites are most often represented by crushing wounds, which makes it difficult to process. Damage is localized mainly on hand and forearms and in 2/3 cases are accompanied by the development of infection. Approximately 75% of cases infection is caused by Pasteurella SPP representatives., Among other pathogens - a wide range of aerobic and anaerobic microorganisms. Feline scratch disease can occur on the spot of a cat or a scratch or scratch. The infection is called Bartonella Henselae and is manifested by the occurrence of erythematous papula (as a rule, after 3-10 days after injury), regional lymphadenitis and general infectilation symptomatics. The disease is permitted after 2 months, however, in some cases, the development of pneumonia, encephalitis or hepatitis, rarely pathology of the organ of sight may be complicated.
Rodents. The bites of small rodents, such as mice, rats, hamsters and guinea pigs, can be contaminated by a number of microorganisms, including Pasteurella SPP representatives. and Streptobacillus Moniliformis (causes «Feathery of rat bite»). Bite protein presumably can lead to infection with a typhoid or tularemia.
Other animals. Bitches of horses, donkeys, pigs and sheep can be infected with representatives of Acinetobacillus SPP., Pasteurella SPP., staphylococci, streptococci and anaerobic bacteria. Ferree bites Contamined by Staphylococcus aureus. With bite of bats, rabies are transmitted. Camel bites lead to infection by PSeudomonas SPP representatives., staphylococci and streptococci, as well as Clostridium Tetani. Monkeys bites are infected mainly by bacteroids, fuzobacteriums, staphylococci, streptococci and E.withrodens. Herpes B (Herpesvirus Simiae), leading to the development of rapid progressive encephalomyelitis, which reaches 70%, can be transmitted with the Makak bite.
Diagnosis and treatment of wounds from bites
In the initial handling, anamnesis is harvested (the bite time and view of the animal), the fence of smears for bacteriological research and primary surgical processing of the wound. In the presence of systemic signs of infection, blood is also carried out to detect aerobic and anaerobic pathogens. In the contamination of wounds by soil, vegetable fragments or water from ponds, lakes, aquariums, as well as patients with immunodeficiency states, bacteriological research on mycobacteria and mushrooms. When a person bite, it is also necessary to conduct an examination for infection with the hepatitis B virus and HIV. Other clinical and instrumental studies are performed according to indications (for example, radiography or ultrasound, with suspected involvement in the bone, joints or the presence in the wound of the foreign body).
Wound treatment lies in washing with saline or water, with shallow damage it is possible to use antiseptics (hydrogen peroxide or poveney iodine). Easying of the Russian Academy of Sciences is recommended for fresh (less than 6 hours) presumably not infected processes, as well as for cosmetics (on face). The delayed breaking of the wound (after 3-5 days) is used in bite for more than 6-8 h, localized in the region of the limbs and accompanied by the scarmers of tissues.
Indications for hospitalization are fever, sepsis, progressive cellulite, expressed edema or tissue damage, loss of limb function, immunodeficiency condition of the patient, as well as infection with hazardous infections (for example, Herpesvirus Simiae), in which patients should be kept in quarantine.
The purpose of prophylactic antibacterial therapy is shown in the bite of man, cats or complicated dog bite, as well as during the localization of the process in the field of limbs, genitals and persons, a heavy degree of damage, involvement in the pathological process of bones and joints or localization of the bite near the prosthetized joint and in patients with immunodeficiency patients. states of various origins.
The choice of antibacterial drug is carried out on the basis of data of bacteriological research. Prior to obtaining its results, the drug selection is amoxicillin / clavulanate (625 mg 3 times a day for adults). With allergies on penicillins, it is possible to prescribe a metronidazole in combination with doxycycline when cat bite and dogs. In human bites, metronidazole can also be used in combination with erythromycin, but the use of ciprofloxacin in combination with clindamycin can be preferable. With a serious nature of infection, antibiotics are entered intravenously, the duration of therapy depends on clinical dynamics.
Preventive antiviral therapy (hepatitis B virus, HIV, rabies and Herpesvirus Simiae) are carried out in suspected the possibility of infection according to standard schemes. The prevention of the tetanus (anticipable vaccine and anticipable immunoglobulin) is carried out in the absence of a patient confirmed immunological anamnesis (T.E. data and timing of the planned immunoprophylaxis of tetanus). If there is a risk of infection with hepatitis or HIV, the patient's observation should continue at least 3 months.