Systemic red lupus - very heavy and not so rare disease. Its treatment is a labor-intensive occupation, patients have a long time in the hospital and get enough aggressive therapy. What is red lupus? Why does it arise and givend to cure? This article is responsible for these and other questions.
Content
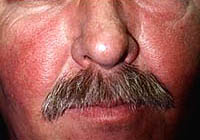
The name is due to the fact that it was originally in 1872, a skin disease was described, which was called «Red Volcanka» – Abundant bright red rash corrosed the skin, especially on the face, which reminded the wolf bites («lupus» maybe by the way not only «Red», But tuberculosis, with skin tuberculosis).
Subsequently, it turned out that «Red Volcanque» Along with the skin, joints, heart, kidneys, central nervous system and other organs, and other organs, in connection with which the name appeared «Systemic Red Volchanka», or SCB.
As for the causes of this disease, there is no single reason. In the development of the disease, the main role belongs to violations of the immune system. Normally, immune responses are aimed at destruction of alien for the body of agents – bacteria, viruses, as well as own cells – aged, damaged or mutating, that is, changed under the influence of any reasons for their properties. Some cells of the immune system produce proteins that recognize and «Capture enemy», Other this «Related enemy» surround I «eat».
But in some cases, the immune system begins to perceive as «enemy» Own tissues of the body – skin, mucous membranes, lymph nodes, vessels, kidneys and t.D. The starting mechanism of this failure can be factors such as solar radiation, cooling, stress, injuries, bacterial and viral infections, vaccination, the effects of certain chemicals and drugs.
Big, although there is still not a fully clarified role, there is a high level of female sex hormones, therefore women of childbearing age are most often ill, the disease is often manifested (this does not mean that it is exactly then it arises) after childbirth and abortion.
In terms of cases, the starting mechanism remains unknown, but the above mentioned violations of the immune system, once arising, continue to provide their destructive effect.
Question # 2. Lie SD inheritance? Do they hurt?
SLE is not a hereditary disease, but genetic factors play an important role in its development. Suffice it to say that 5% of patients with SLE have relatives, also suffering from this disease, and single-hour twins fall in 24% of cases. At the same time, responsible for the predisposition to this disease is not one specific gene, but many different genes, therefore the probability of inheritance is small.
The disease can develop in childhood, but it happens quite rare, most often, as we have already mentioned, young women are ill.
Question number 3. Why do you need to take so many complex analyzes and is it necessary to make kidney biopsy?
Each disease has its own characteristic features, its «face», called physicians «Clinical picture». When SLE for such signs set – These are typical skin changes, joint pain, long-term increase in temperature, increasing lymph nodes, kidney damage, central nervous system, blood change and T.D. These symptoms may occur in various combinations. But it is well known that similar symptoms may be observed in some other diseases – oncological, hematologic, infectious. This is – so called «Masks» Diseases.
In order to confidently determine the diagnosis of SLE and eliminate other reasons, a laboratory survey must be carried out. The combination of characteristic symptoms with positive data of laboratory tests allows you to diagnose with an accuracy of 99%. Investigate blood for the presence of autoantibheus, that is, specific proteins forming complexes with their own tissues of the body and damaging these fabrics.
Antibodies to DNA and Anti-Kenetary Factor (ANF) have the greatest diagnostic value. In addition, an important laboratory feature is the so-called «Le-phenomenon», determined by the specific gluing of blood cells. The name comes from the Latin name of the disease «Lurus Erythematosus». In addition to these special laboratory studies, a set of patients with SLE is performed «ordinary» blood tests and urine. This is necessary in order to correctly assess the situation at various stages of treatment.
As for the biopsy of the kidney, it is necessary not so much for the diagnosis (although in some cases the diagnosis of SD is raised according to the biopsy of the kidney), how much to determine the tactics of treatment. The fact is that more than 80% of patients with SPV have a kidney defeat. The severity of this lesion is very different, but to know how much the kidney tissue is damaged, only by considering this fabric under the microscope, that is – After performing biopsy.
Meanwhile, it is a lupus nepritis (kidney damage) is one of the most serious manifestations of SD and requires the most aggressive treatment. Therefore, the kidney biopsy helps to determine the doses of drugs, the mode of their introduction and the duration of the main course of therapy.
Question number 4. Is it impossible to do without hormones and chemotherapy? And why medications need to take so long?
In cases where it comes not to skin form, but about the systemic red loll, when there is a damage to the kidneys, the central nervous system, the heart, lungs – do without immunosuppressive, that is, the overwhelming immune responses, therapy, it is impossible. SLE refers to the discharge of diseases in which the treatment must be carried out.
Up to the middle of the twentieth century, before the introduction into the clinical practice of corticosteroids (hormones, one of which is prednisone), the SLE refer to the category of diseases with a hopeless forecast. Prednisolone suppresses immune responses and thereby reduces the activity of the disease to a minimum. Its application allowed to save the lives of many thousands of patients with SLE.
Prednisolone treatment is starting immediately after the diagnosis is established and carried out very long. And the dose of the drug must be high. If the dose or the duration of treatment is insufficient, then either the improvement will not come at all, or after the improvement period (this is called the remission) will develop an aggravation.
But one prednisone is not enough. For successful treatment requires the use of drugs called cytostatics. Literally this name is translated as «stopping cells». With regard to SKV, it is about the impact on the cells of the immune system. Cyticostatics began to be used since the 70s of the XX century, as a result of which the survival of patients with SD increased to 90%.
In addition, the use of cytostatics allows to reduce the dose of prednisolone, which means its side effects. What kind of cytostatic and in what form to appoint – The specialist doctor is solved on the basis of a comprehensive examination, including biopsy data kidney.
Question number 5. What to do to not add in weight, taking prednisone? Is it possible to completely cancel this drug over time?
Prednisolone – This is a hormone similar to natural cortisol. Cortisol is produced by adrenal glands and has a wide range of action. It participates in the regulation of water-salt, carbohydrate, protein and fat metabolism, ensures the maintenance of blood pressure, has anti-inflammatory, antioallergic and immunosuppressive (i.e. suppressing immune responses).
In the wells, as well as a number of other diseases, such as bronchial asthma, rheumatoid arthritis, chronic glomerulonephritis, therapeutic effect is achieved due to immunosuppressive, anti-inflammatory and anti-allergic effect of prednisolone.
Impact on metabolism, as well as irritant effect on the gastric mucous membrane, are side effects. It is completely impossible to avoid them, because the therapeutic doses of prednisolone significantly exceed the natural level of cortisol in the body, but when compliance with the necessary precautions can be reduced by side effects to a minimum.
 First of all, the patient receiving prednisone must periodically pass the survey of the stomach – Gastroscopy. To protect the mucous membrane, enveloping drugs are prescribed, such as an almagel, as well as drugs that reduce the acidity of gastric juice (Ranitidine, Famotidine, etc.).
First of all, the patient receiving prednisone must periodically pass the survey of the stomach – Gastroscopy. To protect the mucous membrane, enveloping drugs are prescribed, such as an almagel, as well as drugs that reduce the acidity of gastric juice (Ranitidine, Famotidine, etc.).
For the prevention of disorders of the water and salt metabolism, especially patients with kidney damage, it is necessary to rigidly observe the inset diet. Otherwise, prednisolone will delay the sodium in the body (and the cook salt, as we must remember from the school course of chemistry, – This is a sodium chloride), and after it and water. Because of this, especially at the initial stages of treatment, when the anti-inflammatory and immunosuppressive effect has not yet come, swelling may occur and the blood pressure increases.
An abolishing diet implies a complete exclusion of food cracking in the cooking process, which means that it is necessary to abandon meat, fish and vegetable canned food, sauces, marinades, pickles, smokers, mineral water, as well as sausages and cheese. Food cooked houses will not solisfts at all.
To prevent the obesity and development of diabetes mellitus, it is necessary to eliminate easily durable carbohydrates (sugar, candy, chocolate, pastries, pasta) and animal fats (butter, oily meat).
The question immediately arises – And what then is there? Fruits, vegetables, cottage cheese and dairy products, cereals, low-fat meat, sea fish. By the way, their consumption will protect the musculoskeletal system from the effects of prednisolone on the exchange of potassium and calcium.
As for the abolition of prednisone, then seek not to this. The fact is that the SLE is not so much a disease as lifelong condition. This refers to the state of the immune system, which, being at the beginning of the disease, is tuned against its own body tissues, retains this mood for many years and decades, even if all this time is preserved clinical and laboratory remission.
Therefore, after the main course of treatment, it is necessary to constantly carry out the so-called «Supporting therapy», Otherwise, the probability of exacerbation increases many times. Supporting therapy includes prednisone in small doses (0.5-2 tablets per day) and, in some cases, cytostatics, also in small doses.
Supporting therapy has minimal side effects, but, of course, should be conducted under the supervision of specialists. Thus, patients with SLE should be observed at the rheumatologist or the nephrologist for life. Independent cessation of treatment is unacceptable.
Question number 6. Can I continue to work, learn? Whether disability is obligatory at SP?
During the period of the activity of the disease, when the main course of treatment is held, occupying at least six months, and most often 10-12 months, it is necessary for a long stay in hospital, repeated hospitalization. Modern immunosuppressive therapy requires strict medical control.
In addition, immunosuppression suppresses not only pathological immune reactions, but also normal immunity, therefore patients receiving prednisone and cytostatics in therapeutic doses, are susceptible to any viral and bacterial infections. And this means that for the prevention of complications, it is necessary to minimize the trip in transport, staying in places of cluster of people.
Therefore, at the time of the main course of treatment, work and school must be interrupted – at least for a year. Usually, the II group of disability is issued. Subsequently, when remission of the disease and the transition to supporting treatment, ability to be restored (of course, severe physical work and occupations associated with professional hazards are excluded).
Question number 7. Is it possible to give birth to patients with SLE?

Pregnancy and childbirth at SLE increase the risk of exacerbation of the disease. Some forms of this disease themselves lead to miscarriage and non-dischanging pregnancy. In addition, the reception of some cytostatics can cause the development of congenital pathology of the fetus. Therefore, pregnancy for patients with SLE is undesirable.
However, in cases of long-term resistant remission, against the background of receiving small doses of prednisolone and drugs, preventing related miscarriage, under the permanent monitoring of specialists, pregnancy is possible. In particular, we have been observing several patients for many years, safely giving birth to healthy children and remaining in remission.
In conclusion, I would like to emphasize once again that the SLE refers to the category of diseases in which timely correctly selected treatment radically changes the fate of patients and allows you to extend a full-fledged life for decades. Of course, under regular medical supervision and subject to strict adherence to all recommendations.