Some believe that scars decorate a man. For someone they make a man more sexy, for someone more brave, strong...
Content
Scars and scars are essentially the same thing. Scars are the domestic name of the scars. In medicine it is believed that the scars are the result of replacing the skin's own tissues on the connecting result of various damage: mechanical impact, temperature (scars are formed after burns), skin diseases (the so-called pedestal). The problem of scars is generally both for doctors - dermatologists and surgeons - cosmetologists. Each of these specialists is engaged in this problem. Scars are not so simple, as it seems at first glance. There are many subspecies and groups. For example, it is important to separate physiological scarring and pathological. Physiological - this is when after injury, the scar gradually pale and becomes compact. And sometimes suddenly the reverse process begins - the scar increases, it becomes brighter, blushes or blue. In this case, pathological scarring is developing, and then it is necessary to intervene a specialist to make a decision on the correction of the process.
Formation of scar
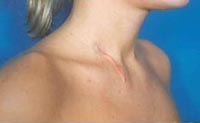 It is very important to understand at what stage of the formation of the scar you turned to the doctor. The success of treatment largely depends on the time of the emergence of the problem: the sooner, the better. There is a big misconception, as if from scars it is possible to get rid of forever. No, It is Immpossible. Surgeon can improve the quality of the scar. Imagine that the scar is wide and rude. An experienced surgeon can make it subtle and less noticeable. It excised excess skin and will form a new one, but more beautiful scar. Cosmetologists and dermatologists can recommend a complex of treatment of scars depending on their species.
It is very important to understand at what stage of the formation of the scar you turned to the doctor. The success of treatment largely depends on the time of the emergence of the problem: the sooner, the better. There is a big misconception, as if from scars it is possible to get rid of forever. No, It is Immpossible. Surgeon can improve the quality of the scar. Imagine that the scar is wide and rude. An experienced surgeon can make it subtle and less noticeable. It excised excess skin and will form a new one, but more beautiful scar. Cosmetologists and dermatologists can recommend a complex of treatment of scars depending on their species.
The scar may occur after injury, operation, piercing and so on and is the result of the closure of the tissue defect of the newly formed by the connective tissue. If the damage affects only the epidermis, the traces does not remain, since the cells of the basal layer of the epidermis retain the ability to fully regenerate throughout life. If the damage affects the deeper layers of the skin (dermis), then the tissue defect is filled with a granular tissue, which is subsequently formed into the scar. With the normal course of the scarring process, the scar fabric is gradually compacted and acquires the color of the surrounding tissues (normal-pic scar). Whether the course of the process is disturbed, then the likelihood of the formation of pathological scars is great.
Types of scars
It is very important to correctly determine the type of scar to determine the term and selection of the treatment method.
Norhmotrophic scars are on the same level with the surrounding skin, have a pale or body color and have elasticity close to normal tissues. They are most often not bothering the patient. As a rule, they are not recommended to be treated radically, that is, resort to surgery. But this does not mean that they do not need to be engaged. With microdermabrasion or surface (sometimes median) chemical peels, these scars can be made practically imperceptible.
Atrophic scars Located below the level of the surrounding skin and are distinguished by flabbing tissues. A typical example of atrophic scars are Stria (stretch marks). There are many methods for treating this type of scars. Moreover, it should be noted that with aesthetic result, almost all patients remain satisfied with the aesthetic result.
Hypertrophic scars protrude above the surface of the skin are limited to the injured area and spontaneously regressing for two years, although regression can be incomplete. The color of such scars, as a rule, pink. This type of scars is perfectly treatable, and they do not recur. The best cosmetic result is achieved in surgical treatment - excision of scar tissue. If the scar of a small size is perfectly undergoing treatment with peels - chemical, microdermabrasion, laser grinding. Of the conservative methods, good results are achieved at the expense of electric and ultraphone formation with hydrocortisone, lidase, contracturex or injections of hormonal drugs in the scar zone, such as Diprospane or Kenalog.
Keloid scars There may be a star or fan-shaped, to have a type of linear severity, usually protrude above the skin and have a sharp boundary. Often accompanied by itching, pain, burning. Characterized by the ability to constantly increase and relapses after treatment, as a result of which the size of the scar can several times higher than the size of the wound. Treatment of keloid scars still remains one of the most difficult tasks, the effectiveness of treatment and the frequency of relapses is very variable.
Methods of treating scars
Surgical excision of keloid scars in itself is ineffective, as it stimulates additional deposition of collagen and quickly leads to relapse. The introduction of corticosteroids into the scar fabric is perhaps the most applied method. According to some clinical data, its effectiveness reaches 90%, although it is necessary to recognize that sometimes local skin reactions occur in the form of its atrophic or pigment. Only the fact that over time these side effects pass.
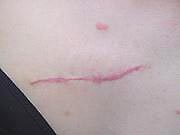 Why it is so important to determine what type of scar belongs to the result? Because it depends on how it needs to be influenced. Atrophic scars appear on the skin due to acne and poor-quality operations on the face - for example, when they poorly removed the mole or papilloma. The task of the doctor - fill the hole that was formed. After all, what is atrophy?
Why it is so important to determine what type of scar belongs to the result? Because it depends on how it needs to be influenced. Atrophic scars appear on the skin due to acne and poor-quality operations on the face - for example, when they poorly removed the mole or papilloma. The task of the doctor - fill the hole that was formed. After all, what is atrophy?
First of all - lack of growth of fabric. In atrophic scars, the formation of collagen is very bad, it lacks it to fill the hole. Externally, such fumes on the skin look like obvious defects that arose after the destruction of the follicle and the surrounding connective tissue, and sometimes the destruction of subcutaneous fiber. Destruction can be so big that scars are deep and wide, which is typical for heavy forms of acne.
Atrophic scars need to fill in special preparations with a hyaluronic acid content. And as it is impossible, chemical peels are suitable for them. As for hypertrophic scars, i.e. scars with an abrasiveness of the fabric, in this case such a scar need to be aligned with the skin surface, that is, make the norm ill-structure. Very well smoothed the manifestation of hypertrophic scars Grinding with a laser and dermabrasion. And the harder to influence the keloid scars. They are extremely difficult to treat them. And they should speak separately.
Mysterious keloid scars
Keloid scars love to pretend hypertrophic. It is very important that the doctor can distinguish one of the other. Otherwise, treatment may not only be unsuccessful, but also dangerous. The keloid heads of doctors became interested in the late XIX century, turning attention to the fact that some scars for a long time after receiving injury develop and further develop the border of damage to the skin. If, in the case of hypertrophic scars, their dimensions clearly correspond to the size of the damage, then in the case of keloids, they can occur at the place of small damage and exceed the primary area several times.
Most often, keloid scars develop on ear sinks, chest, less often - on the joints. Known cases of development of keloid scars on the face.
Development of keloid scars
The development of keloid scarring occurs in four stages:
- The epithelization stage means that the injured area is covered with a thin film of a flat epithelium, after 7-10 days it begins to grown and slightly compacted, its color from pink becomes more pale. In such a state, the scar is 2-2.5 weeks.
- The step of swelling is characterized by an increase in the scar, pain in contact with it, the scar is already towers above the skin level. Through 3-4 finished soreness decreases, and redness increases, acquiring a cyanotic shade.
- The stage of the seal - the scar is condensed all over, focal covered with dense plaques, becomes a bug and outwardly resembles a keloid.
- The stage of softening - the scar pale, becomes soft, movable and painless. The process can go to the softening stage, and the scar will save the keloid character.
On their varieties of keloids are divided into young and old. Tactics of treatment of these two forms are fundamentally different. Young keloids are keloids with a period of existence from 3 months to 5 years. Characterized by active growth, have a smooth shiny surface and color from red to cyanotic. Old keloids are keloids with a period of existence from 5 to 10 years. Characterized by an uneven wrinkled surface, sometimes - the west of the central part, more pale painting compared to young keloids.