Why periodontitis occurs? How to diagnose and treat periodontitis? Answers to these questions will be found in the article.
Content
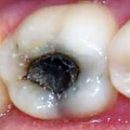
Personontitis is defined as a disease in which the destruction of the teeth supporting apparatus occurs. Periodonts are fabrics that keep the tooth. These include bone, gum, mucous membrane and ligaments. With periodontitis, the infection falls into the space between the tooth and the gums and begins to destroy the root of the root of the tooth with the bone.
100% of the adult population of the Earth and in 80% of children, according to WHO experts, there are one or other signs of periodontitis.
Why periodontitis occurs
Bacteria is constantly present in the oral cavity. They fall to us with food, water, constantly in dental. They are the cause of periodontal diseases. Microbes allocate toxins (poisonous products of life) that destroy the tissues. First soft - mucous membrane and gums themselves. The stage of the disease of the periodontal, when only the mucous is amazed, called gingivitis. The destruction of deeper tissues of the gums, which lead to loosening and loss of the tooth - it is already periodontitis. Microbes penetrate the physiological furrow between the tooth and the gums, forming pathological pockets. These are the tanks of anaerobic infection, that is, developing in depth, without access of oxygen. In such a shelter, nothing prevents microbes to destroy all the fabrics, including bone.
Inflammation, leading to periodontitis, develops with a weakening of the protective forces of the body, with the caries of the tooth, after injury to the tooth (for example, when hitting, microtravoma at the snitch snacking), under the influence of chemicals (acids, alkalis). The cause of periodontitis can also be an allergic reaction to potent drugs. Personontitis sometimes develops with incorrectly furnished fillings or poorly fitted dentures.
What are the symptoms of periodontitis
The disease has acute and chronic stages. Chronic periodontitis, in turn, has a light, medium and serious flow.
 The initial period of the disease is characterized by itching, pulsation in the gums, the mobility of the teeth, the feeling of inconvenience when chewing, an unpleasant smell of mouth. As the process progressing the support apparatus, the tooth is loosened, the mobility of the teeth increases, the necks of the teeth are exposed and acquired increased sensitivity. During food, the food is stuck in interdental intervals, which causes an even greater sense of discomfort when chewing food. Gums become painful, swell, when cleaning the teeth bleed. In the heavy stage, a pronounced pain syndrome occurs, the body temperature rises, weakness, ailment and other. Formed a large amount of dental deposits. Teeth soreness, its increased mobility, or the distribution of inflammation for neighboring teeth violate the processes of food chewing. This creates an additional load on the organs of the digestive tract and may cause their illness.
The initial period of the disease is characterized by itching, pulsation in the gums, the mobility of the teeth, the feeling of inconvenience when chewing, an unpleasant smell of mouth. As the process progressing the support apparatus, the tooth is loosened, the mobility of the teeth increases, the necks of the teeth are exposed and acquired increased sensitivity. During food, the food is stuck in interdental intervals, which causes an even greater sense of discomfort when chewing food. Gums become painful, swell, when cleaning the teeth bleed. In the heavy stage, a pronounced pain syndrome occurs, the body temperature rises, weakness, ailment and other. Formed a large amount of dental deposits. Teeth soreness, its increased mobility, or the distribution of inflammation for neighboring teeth violate the processes of food chewing. This creates an additional load on the organs of the digestive tract and may cause their illness.
For a light degree of chronic periodontitis, the presence of bleeding gums is also characterized; The depth of the gantry furrow is approximately 3-3.5 mm. For chronic periodontitis of moderate severity, the unpleasant smell of mouth, sharp bleeding gum, color change, type of gums, appearance of slots between teeth.
The severe degree of chronic periodontitis is characterized by the appearance of pain in the gums, difficult chewing, displacement and destruction of individual teeth. The pain force to abandon the cleaning of the teeth, which leads to significant deposits of dental plates and stone and aggravates the course of the disease. The depth of pathological pockets exceeds 5-6 mm.
The aggravation of chronic periodontitis is usually associated with a sharp deterioration in the overall condition of the patient (infectious diseases, heart failure, etc.D.). In exacerbation, there is a sharp pulsating pain, an increase in temperature, ailments and weakness. There is a bright redness and bloodyness of the gums, from the seashene pocket is distinguished by pus.
How to diagnose periodontitis
In the presence of one or more symptoms of periodontitis described above, you need to consult a doctor as soon as possible. The most important diagnostic event that helps to recognize the disease is to measure the depth of the gap between the tooth and the gum, the so-called gums. To this end, the dentist uses a special tool (periodontal sample), which is placed between the tooth and the gums and helps measure the depth of the gap.
The depth not exceeding 2-3 mm is a sign of a healthy gum. The depth of more than 5 mm indicates a pathological process. It is very important to assess the hygienic state of the oral cavity (the presence of plane, dental stone). Of the other additional methods, X-ray has the greatest importance, which allows to estimate the state of bone jaw bone.
How to treat periodontitis
The disease requires the urgent intervention of the dentist. Treatment of periodontitis includes non-surgical and surgical methods. The first (professional hygiene) is used in the early stages of the disease and for prevention. They are to remove the tootham (mechanical or ultrasound) and polishing the surface of the tooth, followed by the processing of the crown and the root of the tooth with special brushes with fluorine-containing protective varnish.
There is a deepest dental removal procedure, which is called Kurezh: The doctor removes sediments using special hooks, excavators, curetles (closed cabinage), or if an operation is required, cutting the gums (Open Curetage). In case the depth of the gantry furrow does not exceed 5 mm, as well as during daily oral hygiene, the dental removal is the only recommended therapeutic event.
Another way of surgical treatment is the patchwork method when the upper part of the gums is removed, the roots of the teeth are cleaned, and the flap is sewn into place. The task of surgical methods is to eliminate gum pockets (consequence of bone resorption) in order to the tooth again gained stability.
Since periodontitis is an infectious inflammatory disease, after establishing the pathogen, the doctor will be able to assign you an effective antibiotic. Antibiotics preferred lincomycin, tetracycline, with preliminary check of microflora sensitivity. It should be noted that antibiotics are used in exceptional cases and strictly by testimony.